
Empowering women enhances the health of people, animals and the environment
Our health is improved when decisions include all perspectives; investing in gender-responsive interventions increases the potential for success and leaves no-one behind.
Core message
Facts
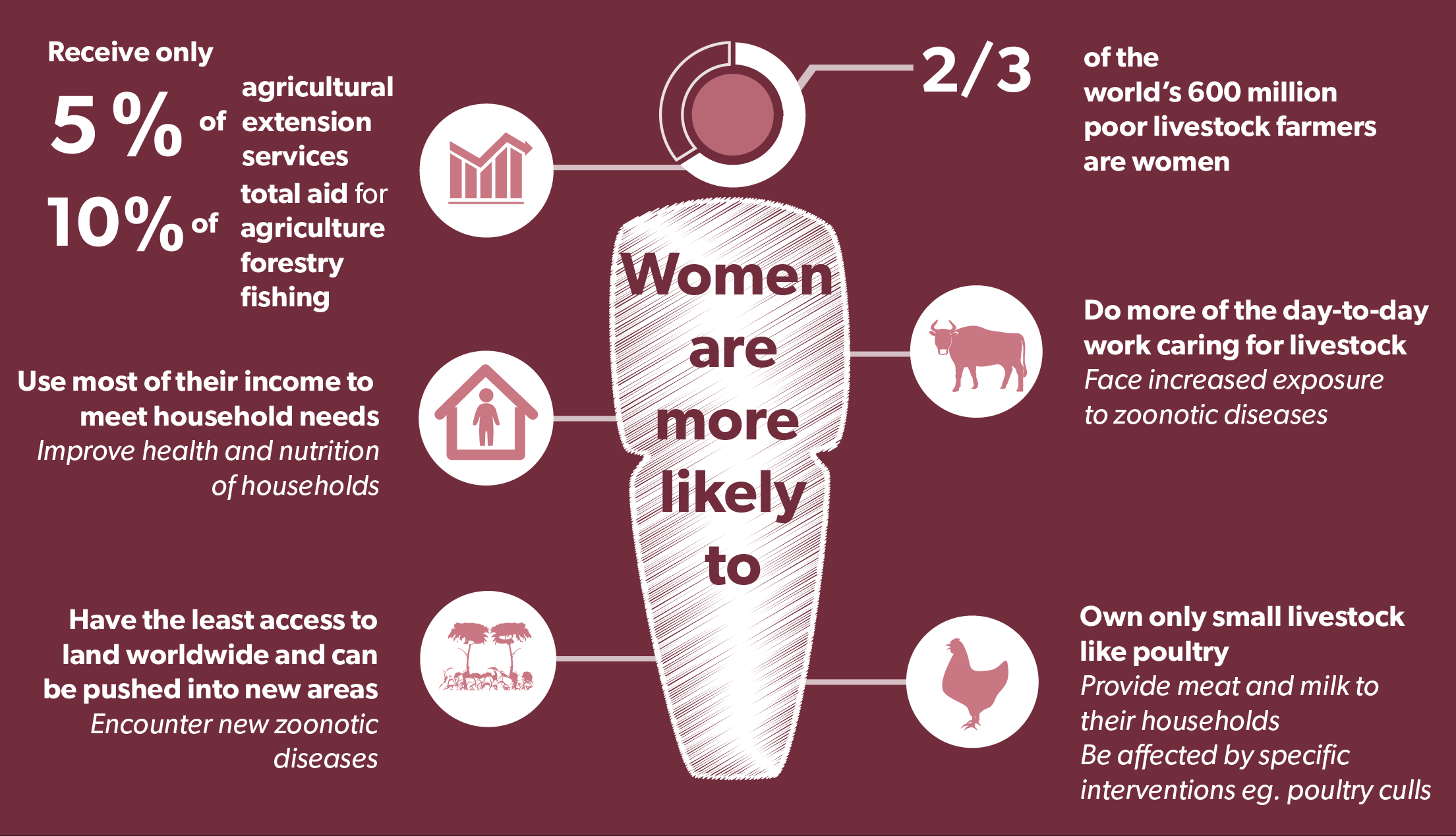
- Women comprise most of the world’s 600 million poor livestock keepers, they prepare most of the world’s meals and they usually attend to important local assets like water and clean environments.
- Ensuring women’s health is itself critical to productive societies. They provide much labour for farming, they spend their income on household and education, and they care for children. Threats to women’s health, or leaving them out of decisions, can have catastrophic consequences.
- Depending on local contexts, culture and norms, and products, women and men dominate or are excluded from different segments of food value chains, exposing them differently to zoonotic and food-borne risks.
- In addition to socio-cultural roles affecting health, men, women, the old, the young and other groups ae vulnerable to different risks and burdens. This is often associated with what they eat; men usually get meat while children and women rely on less nutritious or less healthy animal products.
- Depending on these local contexts, women can be well-paced to play key roles in safer food, environmental health, disease surveillance and control and in improved animal care.
Women and men experience and interact with the world in different ways, resulting from social, economic, political, cultural and other inequalities. Understanding—and sometimes harnessing—these differences helps us tackle problems arising at the interfaces among animal, human and environment health.
Emerging research on gender norms and dynamics and their effects on women’s access to and control over resources, assets, benefits and opportunities points towards promising One Health interventions that address the specific health risks and burdens that women face.
Animal health and care
Women and men have complementary, but distinct, roles in animal health and care. Yet women farmers receive only 5% of all agricultural extension services across 97 countries and only 15% of extension-service providers are women. Only 10% of total aid for agriculture, forestry and fishing goes to women. Overlooking a major class of people risks leaving them behind; it also overlooks their potential as actors for change, uniquely positioned to address cross-cutting health issues.
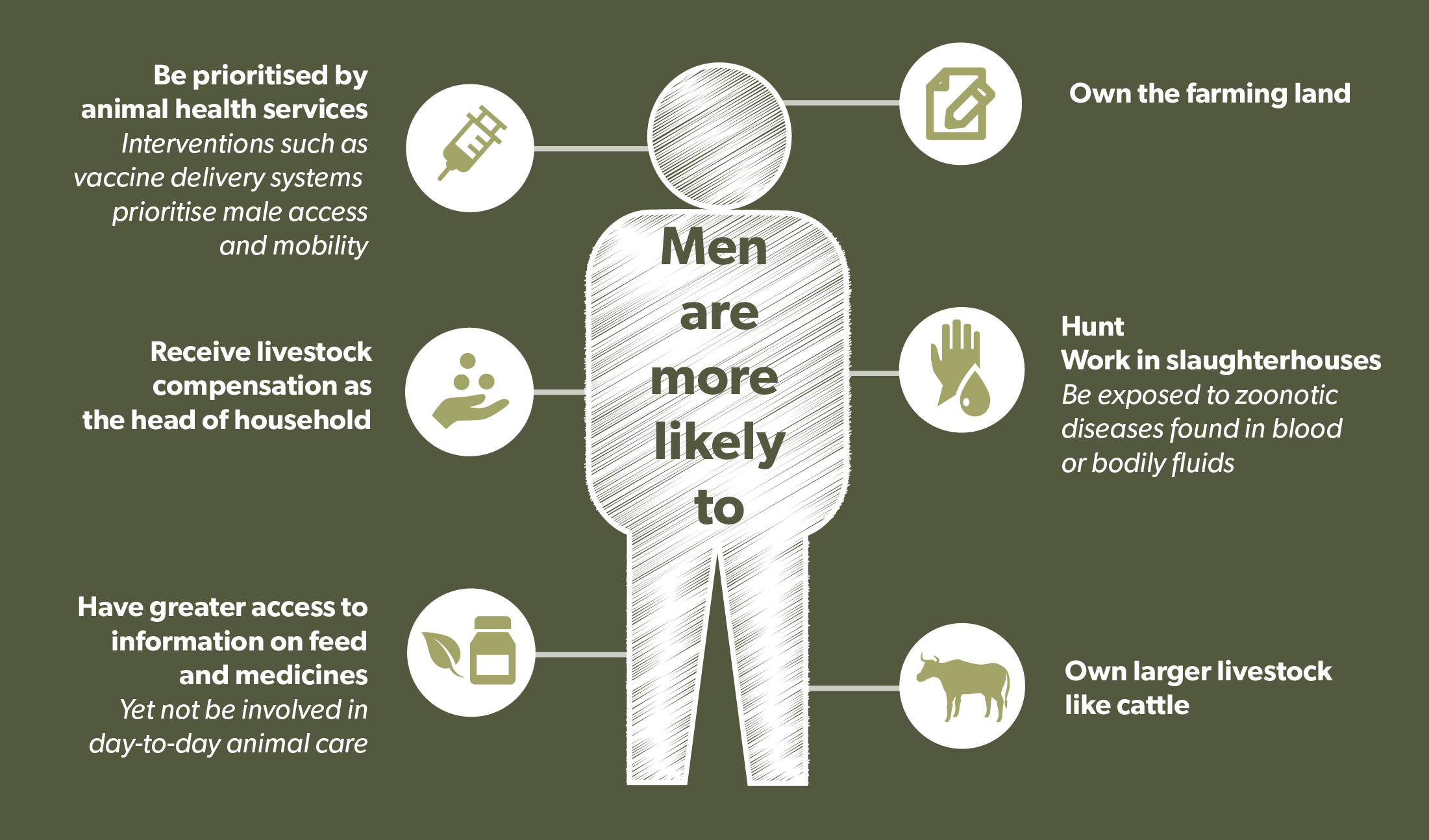
The roles of women and men are determined by socially enforced attitudes and behaviour (gender norms) – with some activities generally reserved for women, or seen as more suitable for women, and others for men. Gender norms have resulted in men most often owning and managing larger animals while women care for poultry and small ruminants such as goats. These gender roles in livestock keeping can be critical for household food security. For example, chicken meat and eggs are important contributors to household income and protein and the loss of birds through illness can be devastating. One Health approaches that appreciate the differences and disaggregate effects and impacts by gender can better target, for example, interventions from agriculture and health ministries.
Access to resources is often highly gendered. Men generally enjoy greater access to information on feed and medicines, though women undertake the day-to-day tasks associated with animal care and can be best placed to implement interventions, spot diseases and ensure prudent use of antimicrobials. Animal health services such as vaccine delivery systems may prioritise men’s activities or unwittingly discourage uptake by women who for gendered reasons such as a lack of mobility can find them hard to access.
Sometimes there is a direct, gendered link in strategies to control disease. Government-mandated culling during avian influenza outbreaks has at times killed more birds than died of the disease. Compensation has been directed to the heads of households, which may not be the person who owns or manages the poultry. In Turkey, avian influenza outbreaks in chickens managed by women occurred after male hunters left the remains of wild duck carcases in the yard.
Gender norms in animal production affect who is best placed to participate in, adopt and benefit from animal health interventions and technologies, to ensure good animal health and care, as well as to prevent the spread of antimicrobial resistance, a growing threat to global health (see section Health - Managing antimicrobial use in livestock farming promotes animal and human health and supports livelihoods).
Diseases from animals
Gendered roles in animal production are a factor in determining who is most exposed to – and so at risk from – diseases that can pass from animals to people (zoonoses).
Consequently, gender dynamics also determine who is most likely to pass these diseases on to others. Studies show these differences in risk are attributable to gender rather than the biological differences of the sexes.
Other gendered divisions of labour affect zoonotic disease risk too. For example, men have often been the first infected in Ebola outbreaks as a result of their contact with primates, sometimes from hunting. Infections in women come later resulting from their gendered roles as care givers, informal and formal health workers and midwives, and because they prepare bodies for burial.
Access to human health services is also gendered.
Food safety
There is a marked difference between women and men in their risk exposure to food-borne diseases that is attributable to differences in their gendered roles in food production, selling, handling and consuming (see section Health - Healthy, well cared for livestock contribute to improved animal, human and environmental health). For example, where men mainly work in slaughterhouses, they are at greater risk of brucellosis or anthrax infection than women as a result of their direct contact with the flesh and bodily fluids of diseased dead animals.
Women can be more at risk of contamination from bacteria such as Campylobacter which cause diarrhoeal disease as a result of handling raw products during food preparation. Women in some cultures are also more likely to eat offal than men, again placing them at higher risk of diarrhoeal disease. Where animal and public health overlap, women are key actors to achieve One Health objectives.
The environment
Environments, resource use and environmental interventions are shaped by gendered practices (see section Health - Integrating livestock and environmental planning can stem disease outbreaks). Poor populations and especially women living in remote rural areas can face greater exposure to disease. Women have the least access to land worldwide and can be pushed into habitats previously unknown to people, putting them at further risk of new zoonotic disease.
Women can be overlooked in environmental interventions, yet they often have specialist knowledge of indigenous plants, have key roles in biodiversity conservation and they take care of domestic and community hygiene and environmental health.
COVID-19, a zoonosis, has shown how different groups of people are subject to different risks depending on their gendered roles. Women as care workers or workers in meat processing plants have been most exposed to the disease. It remains to be seen whether gender-based constraints to mobility, access to information and health support will limit women’s access to COVID-19 vaccines when these are made available in low and middle income countries.
Community conversations have proved successful in raising awareness of zoonotic diseases at a local level and encouraging community members to challenge entrenched gender norms. In these, and other participatory methods, researchers, community leaders, community members and animal health experts sit down together to discuss problems and reflect on experiences and practices and how these might change. The unity of ‘one’ health is achieved by involving a wide spectrum of people and organizations.
What can be done
Acknowledge gender inequity
Listen to women as well as men. When preparing and designing interventions, leaving no voices unheard helps to deliver gender-responsive interventions that also consider trade-offs and synergies across animal, human and environmental health. One Health is about everyone’s health.
Integrate gender into project planning
Build gender into projects from their start to their end points, including in considerations of budget, surveys, personnel, capacity building, risk assessments and monitoring. Every project document should include qualitative and quantitative indicators to measure the gendered impact and explain the gender norms and dynamics affecting change. Gender expertise should be part of One Health efforts. Environmental impact assessments should measure the gendered effect of environmental changes and interventions on people in addition to environmental outcomes.
Research gender and other inequalities
Work with communities to find out how gender norms work. Collect a full range of data disaggregated by sex. We know little about how gender dynamics affect the potentially synergistic gendered impact of animal, human and environmental health. Gender analyses will help to inform gender-responsive interventions and policies across the sectors.
Implement gender-responsive interventions, solutions and policies
Gender-responsive interventions will better target animal health activities, address gendered constraints and leverage opportunities to prevent or treat diseases, and reach and benefit women and men and girls and boys equitably. They will help improve targeting in environmental interventions. Policy on environment protection and zoonotic disease control must be shaped by an understanding of gender norms and dynamics.

